Detect Waste, Abuse and Fraud with Graph Database & Analytics
- Blog >
- Detect Waste, Abuse and Fraud with Graph Database & Analytics
Unfortunately waste, abuse and outright fraud are rampant in the healthcare industry.
Healthcare-related fraud is estimated at around 3-10% of the total cost and is rising, especially with the opioid epidemic affecting over 2 million Americans. In 2017, the Boston Globe uncovered a massive network of brokers who specialize in enrolling multiple patients with phony addresses via healthcare.gov, the portal created for Obamacare or the Affordable Care Act.
These patients are signed up for out-of-state insurance plans and enrolled in treatment centers where the administrators are providing tens of thousands of dollars in kickbacks per patient to the brokers as well as the physicians who refer the patients. In reality, these patients never receive any care from the treatment center, and instead, receive a kickback for participating in exploiting the insurance companies with generous PPO plans.
Finding these fraudulent activities requires analysis of internal data regarding the patients, opioid treatment facility centers, as well as referring physicians and connecting it with external data such as recently used addresses and phone numbers to find the hidden connections among patients, doctors, and the opioid treatment facilities. It also requires benchmarking the end-to-end cost care for every member across a network of doctors and opioid treatment facilities to identify higher than the average cost of care, especially for new insurance policies issued under Obamacare or another government medical care plan.
Detecting Fraud with Deep Link Analysis
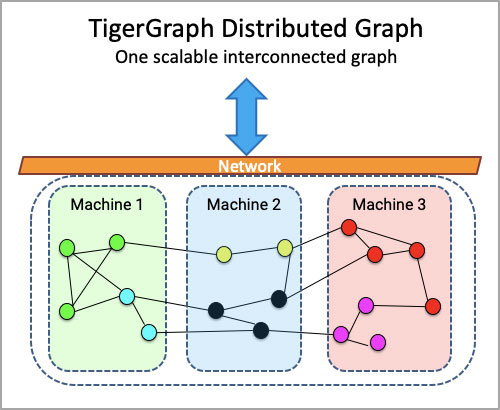
Native parallel graphs, such as TigerGraph, are built to explore and analyze the complex relationships in healthcare data, allowing data scientists and business users to go 10 or more levels deep, across billions of claims and millions of members and prescribers, in real time.
The ability to look penetratingly into large data sets by traversing multiple connections in data is called deep link analysis. Consider a doctor who is referring a large portion of patients to a specific substance abuse treatment center specializing in opioid addiction. At first glance there may not appear to be a connection between the substance abuse treatment center and the doctor and traditional fraud solutions can’t find anything unusual based on the information available for the doctor, as well as the opioid addiction treatment center.
TigerGraph, however, can mine data from third-party sources such as Thomson Reuters or Dunn and Bradstreet to find all known administrators for the drug treatment center and their current and previous addresses. 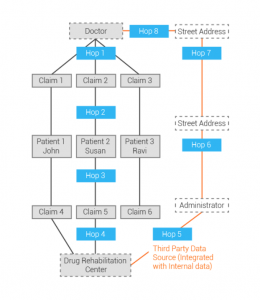
Deep link analysis can uncover collusion between a prescriber and a treatment facility
Identifying Fraud with Hub and Community Detection
Another way for a healthcare payer to spot fraud, abuse or waste is with hub and community detection – this refers to data connections which are tied to one specific entity. Hub and community detection has two steps: the first step is finding the most influential prescribers (hubs) driving maximum referrals for a specific health condition such as cardiac care or diabetes management or a particular type of drug or healthcare treatment; the second step is establishing a community of connected prescribers and the members availing the services from the prescribers.
The next step is establishing multiple communities of connected prescribers and understanding the healthcare products and services consumed by each community so that we can start to benchmark and compare the average cost of care for a specific health condition such as treatment of type 2 diabetes or managing hypertension or high blood pressure.
Using TigerGraph, the healthcare payer can start to understand which doctors have above average spend for the cost of care for similar members, and these insights can be another tool in the toolkit of investigators looking for fraud or waste.
Don’t Be A Victim
There’s never been a better time to upgrade to TigerGraph – healthcare organizations that have done so are already improving the cost of care by identifying nefarious practices and taking steps to eliminate them. You can read reviews of our technology here.
TigerGraph Cloud enables everyone to get started in minutes, build a solution in hours and deploy it to production in days. There’s no hardware to buy and manage, easy integration and scaling, and you pay as you go. There are over a dozen starter kits on TigerGraph Cloud so that you can get going faster. You can review these starter kits here.